Presented by Henry Foong
Ipoh, Malaysia
Ipoh, Malaysia
O/E: Pertinent findings: bilateral and symmetrical erythematous macules and plaques on the dorsum of the PIP, DIO and MCP jpints. They have a violaceous hue and were non tender. Erythematous discoloration was noted
bilaterally and symmetrically around the eyes, nose and forehead.
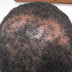
Photos:



Lab:
TWBC 5,500
CK 41 U/l (<201) style="font-weight: bold;">Clinical Diagnosis: Dermatomyositis in Ca stomach
Could this be amytrophic dermatomyositis?
ANA + 1:320 Speckled and homogeneous
Questions: How would you proceed? Would you do a skin biopsy?
Would you treat her? Oral prednisolone or plaquenil alone?
Reference: (from eMedicine.com) Dr. Jeff Callen
Dermatomyositis sine myositis, also known as amyopathic dermatomyositis, is diagnosed in patients with typical cutaneous disease in whom no evidence of muscle weakness exists and in whom serum muscle enzyme levels are repeatedly normal for a 2-year period in the absence of disease-modifying therapies such as corticosteroids, immunosuppressive agents, or both. When studied, some patients with amyopathic dermatomyositis have abnormal ultrasound, MRI or magnetic resonance spectroscopy, or muscle biopsy findings. These patients have muscle involvement, and their condition may be better classified as hypomyopathic dermatomyositis. Patients with these variations may also reflect an underlying malignancy, and some develop severe pulmonary disease, particularly persons from Asian countries.
Patients exist in whom myositis resolves following therapy but whose skin disease remains as an active, important feature of the disease. These patients are not classified as having amyopathic dermatomyositis, despite the fact that, at this point in time, the skin is the major and often only manifestation of the disease. Sontheimer has suggested the term postmyopathic dermatomyositis for these patients.
Therapy for the cutaneous disease is often difficult. Patients who present primarily with skin disease (amyopathic dermatomyositis) and those in whom the muscle component is controlled but who still have significant skin disease exist. The first-line of therapy is recognizing that the patient is photosensitive and advising the patient to avoid sun exposure and to use sun protective measures, including broad-spectrum sunscreens. Hydroxychloroquine and chloroquine have been beneficial in small open-label case studies. Methotrexate is also useful. Mycophenolate mofetil has been reported to be useful. IvIg not only benefited the muscle but also cleared the skin lesions in the patients in whom it was used. Rituximab has been used for skin disease, but the results are mixed. Efalizumab has been used and may have some benefit. Efalizumab (Raptiva), a drug indicated for psoriasis, is being withdrawn from the US market and will no longer be available after June 8, 2009, because of potential risk for progressive multifocal leukoencephalopathy (PML). PML is a rapidly progressive infection of the central nervous system caused by the JC virus that leads to death or severe disability. Demyelination associated with PML is a result from the JC virus infection. JC virus belongs to the genus Polyomavirus of the Papovaviridae.














0 comments:
Post a Comment